Retinal Vein Occlusion — What It Is, What Happens, and What Can Be Done
Retinal vein occlusion is a blockage in one of the veins draining blood away from the retina. When a vein becomes blocked, it creates a traffic jam — pressure builds upstream, and blood leaks out into the surrounding retinal tissue. That leakage, particularly when it reaches the central retina, causes the macula to swell. The resulting macular oedema is what reduces vision.
It usually presents as a sudden change in vision in one eye — blurring, distortion, or a patch of reduced vision that appears over hours to days. It is not painful, which sometimes leads people to delay seeking assessment. Early treatment matters.
RVO doesn't hurt, and that's part of the problem. Patients sometimes wait days hoping it will settle, when in fact those days matter.
Dr Hunt's PhD research at the Save Sight Institute, University of Sydney focused on retinal vein occlusion outcomes, and his ongoing work through the Fight Retinal Blindness! registry continues to examine how RVO behaves in real-world clinical practice.
What Are the Types of Retinal Vein Occlusion?
The type of RVO depends on where in the vein network the blockage occurs.
Branch Retinal Vein Occlusion (BRVO)
The blockage occurs in one of the smaller branch veins draining part of the retina — usually one quadrant or sector. Only that portion of the retina is affected, though if the leakage reaches the macula, vision can still be significantly reduced.
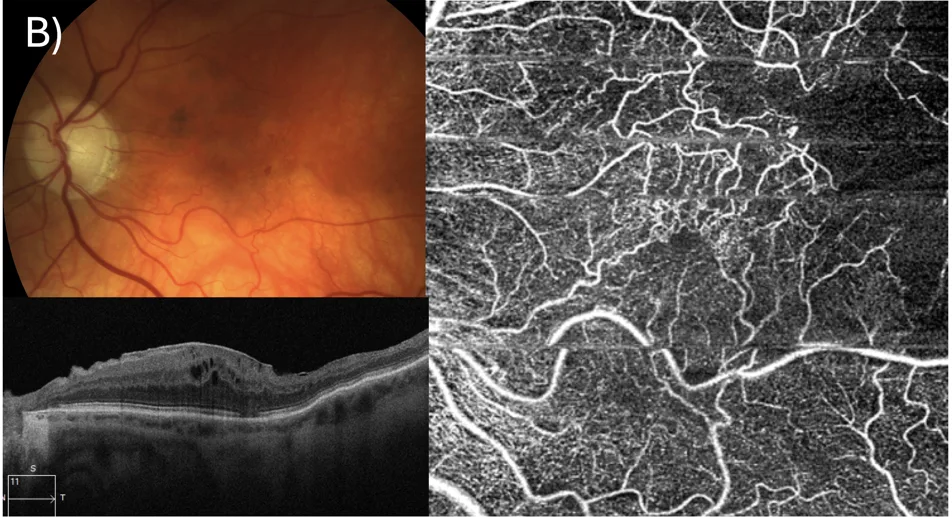
Central Retinal Vein Occlusion (CRVO)
The blockage occurs at the central retinal vein — the main drainage trunk for the entire retina. Because the whole retina is affected, haemorrhage and swelling tend to be more widespread.
Hemiretinal Vein Occlusion (HRVO)
A vein draining either the upper or lower half of the retina is blocked, due to an anatomical variation at the point where the vessels enter the eye. It sits between BRVO and CRVO in terms of the area affected.
What Are the Symptoms of Retinal Vein Occlusion?
- Sudden blurred or reduced vision in one eye
- Distortion — straight lines appearing bent or wavy
- A dark, grey, or smudged patch in the centre of vision
- A shadow affecting part of the visual field
Symptoms develop over hours to days and affect one eye only. Because the other eye compensates, some people don't notice the change immediately — particularly if the affected area is away from the very centre of vision. If you cover each eye separately and notice a clear difference, that warrants prompt assessment.
Act Promptly
A sudden change in vision in one eye should be assessed urgently. Contact the rooms for a same-day or next-day appointment. If it is after hours, present to Sydney Eye Hospital emergency.
What Happens Over Time?
In many cases, the eye gradually develops its own bypass around the blockage. Once that happens, the swelling often reduces or resolves — and many patients can reduce or stop treatment over time.
But this process takes months to years, and waiting without treatment risks permanent macular damage. The role of injections is to control the swelling while the eye does its own repair work. Ongoing monitoring determines when it is safe to extend or stop.
How Is Retinal Vein Occlusion Treated?
Intravitreal injections
The main treatment for RVO-related macular oedema is intravitreal injection therapy. Anti-VEGF medications reduce the leakage and swelling driving the vision loss, and in some cases a steroid implant is used where anti-VEGF response is insufficient. Treatment is started promptly and the schedule adjusted based on how the retina responds at each visit, guided by OCT imaging.
Some eyes need frequent injections to maintain control; others respond well and can extend to longer intervals relatively quickly. The agent and the schedule are matched to how each eye is behaving.
What to expect from eye injections →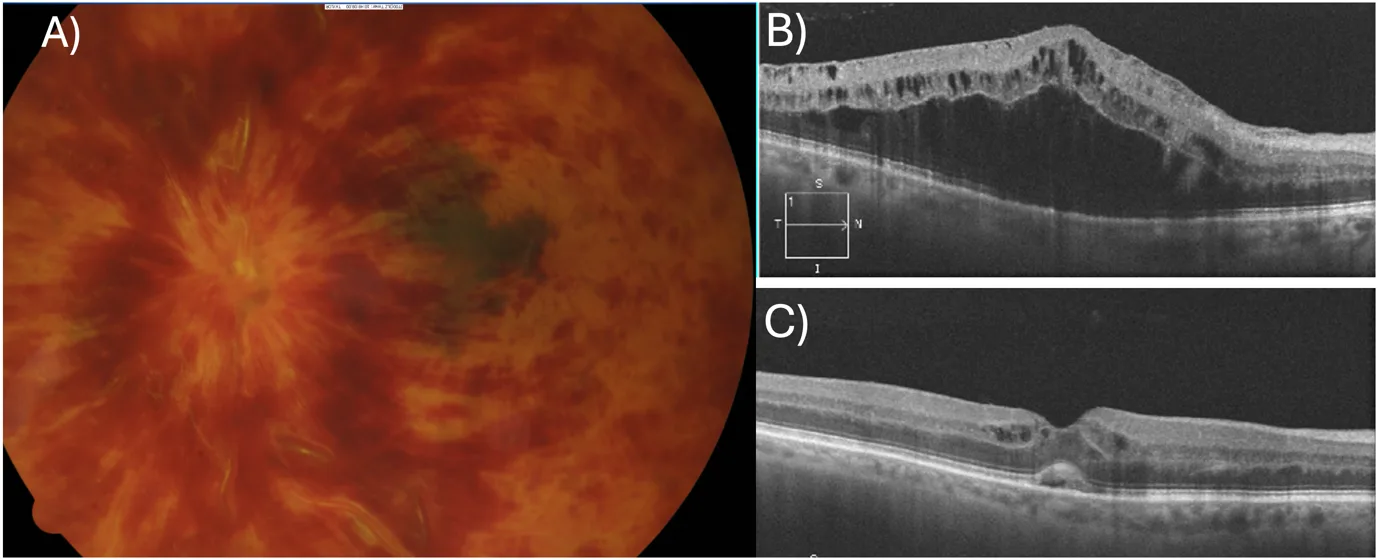
Laser treatment
In the same way that diabetic retinopathy can starve areas of the retina of oxygen and trigger the growth of abnormal new blood vessels, RVO can also cause significant ischaemia — areas of retina deprived of adequate blood supply. When this occurs, abnormal vessel growth can follow, with risks including bleeding into the eye and, in severe cases, a painful form of raised eye pressure called neovascular glaucoma.
Laser treatment to the affected areas of retina reduces the oxygen demand and helps prevent these complications. It does not restore vision but plays an important role in protecting the eye when significant ischaemia is present.
Can I Have Cataract Surgery If I Have Retinal Vein Occlusion?
Yes. Many patients being treated for RVO also develop cataract, and the two conditions can be managed together. Dr Hunt is the senior author of a study using Fight Retinal Blindness! registry data demonstrating that cataract surgery can be performed safely in eyes receiving intravitreal injections for RVO, with meaningful gains in overall vision — though a temporary increase in injection frequency may be needed in the period around surgery to manage any inflammation-related increase in macular swelling.
This is something that can be planned for when both conditions are present.
What to expect during cataract surgery →Research in Retinal Vein Occlusion
Retinal vein occlusion was the focus of Dr Hunt's PhD at the University of Sydney, conducted through the Save Sight Institute. His ongoing research through the Fight Retinal Blindness! registry examines long-term visual outcomes of intravitreal therapy for RVO in real-world practice — the patients seen day to day in a consulting room, not a selected clinical trial population.
This work contributes to understanding treatment patterns, which patients are likely to need ongoing injections, and how factors like treatment consistency affect vision over time.
See Dr Hunt's publications →Retinal Vein Occlusion Assessment
Dr Hunt's PhD focused on retinal vein occlusion outcomes, and RVO remains a particular area of clinical and research interest. New assessments, urgent reviews, and ongoing injection treatment are available at Eye Surgeons Miranda — urgent appointments are prioritised when symptoms suggest a new or worsening RVO.
Frequently Asked Questions — Retinal Vein Occlusion
What are the symptoms of retinal vein occlusion?
Retinal vein occlusion typically causes sudden blurred or reduced vision in one eye, distortion where straight lines appear bent, a dark or grey patch in central vision, or a shadow affecting part of the visual field. Symptoms develop over hours to days and are not painful. Any sudden change in vision in one eye should be assessed urgently.
Can I have cataract surgery if I have retinal vein occlusion?
Yes. Cataract surgery can be performed safely in eyes receiving intravitreal injections for RVO, with meaningful gains in overall vision. A temporary increase in injection frequency may be needed around the time of surgery to manage any inflammation-related increase in macular swelling. This is something that can be planned for when both conditions are present.
How is retinal vein occlusion treated?
The main treatment for RVO-related macular oedema is intravitreal injection therapy with anti-VEGF medications, which reduce the leakage and swelling driving vision loss. Treatment is started promptly and the schedule adjusted based on how the retina responds at each visit. Laser treatment is used in some cases where significant retinal ischaemia is present.
