Pterygium Surgery in Miranda
In the Sutherland Shire, being outdoors is part of everyday life. Time at the beach, surfing around Cronulla, boating, gardening, and outdoor work all add up to years of sun and wind on the surface of the eye — which is why pterygium and other sun-related changes are so commonly seen in this area.
A pterygium is a wing-shaped growth that starts at the inner corner of the eye and slowly extends across the white of the eye and onto the clear cornea. It does not go away on its own, and if it grows far enough it can start to affect vision.
Dr Adrian Hunt performs pterygium surgery as a day surgical procedure using conjunctival autograft — the technique with the strongest evidence for reducing recurrence.
What Is a Pterygium?
In some people a pterygium remains small and stable for years. In others it grows progressively, particularly if UV exposure continues.
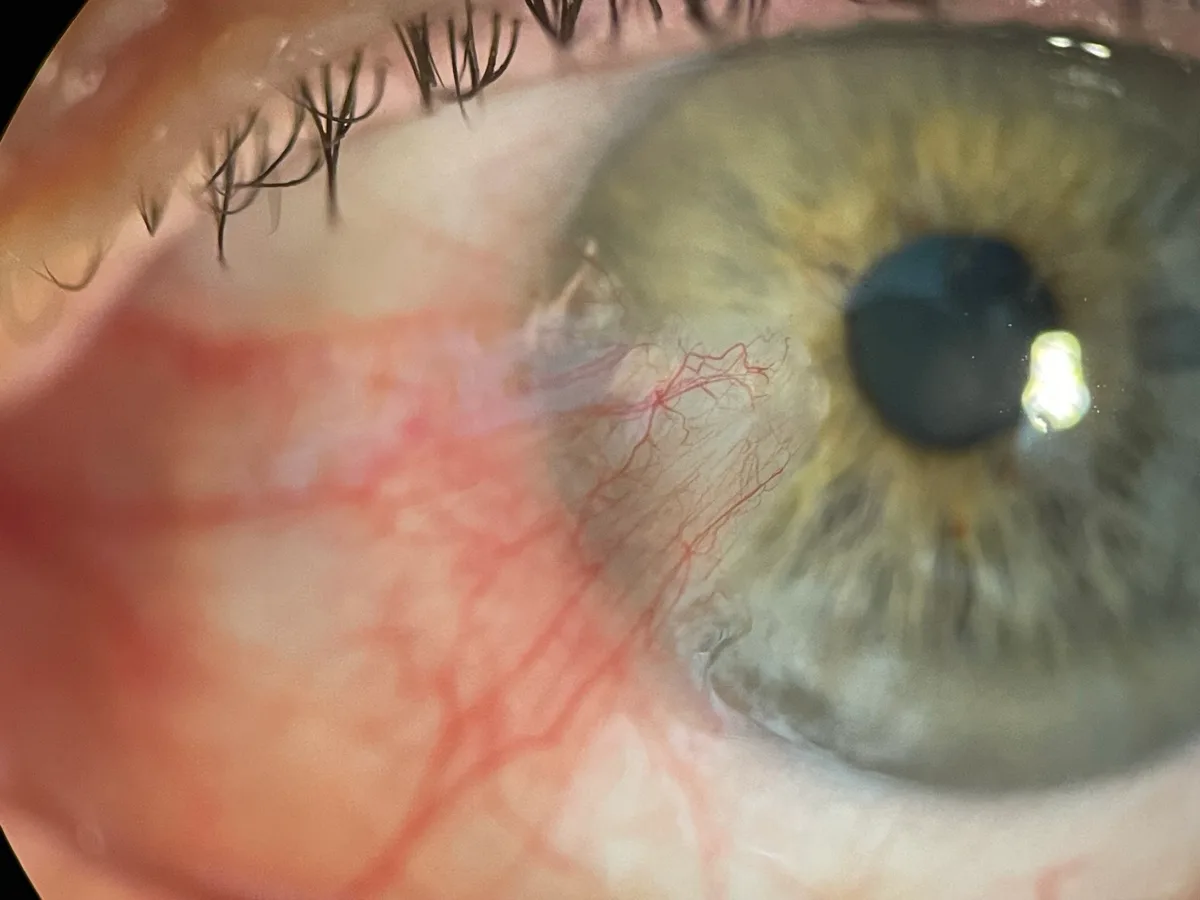
As it grows, a pterygium can:
- Cause chronic irritation, redness, and a gritty sensation
- Induce astigmatism by distorting the corneal surface — affecting vision even when it is not yet close to the visual axis
- Interfere with contact lens wear
- Block the visual axis if allowed to grow far enough across the cornea
- Complicate cataract surgery planning if it distorts corneal measurements
Is It a Pterygium or a Pinguecula?
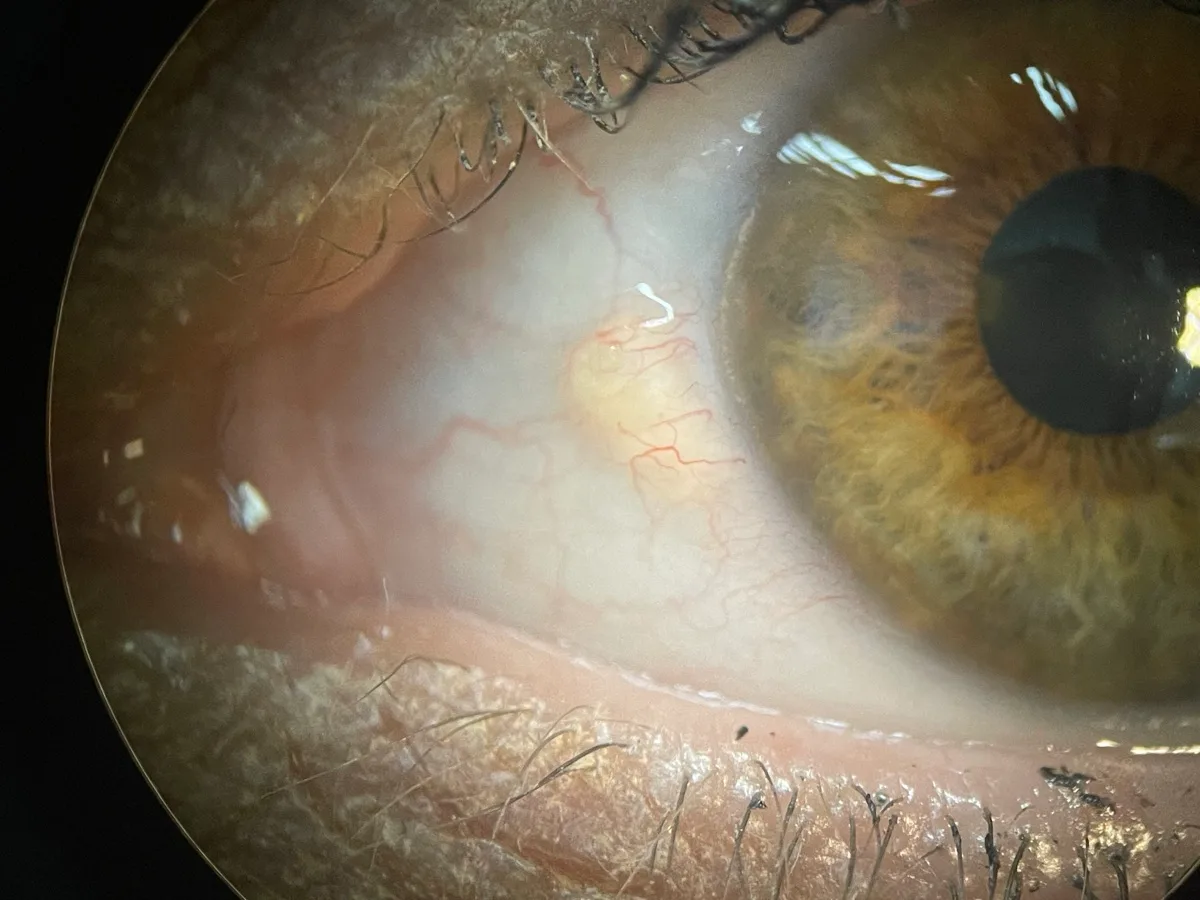
Many people come in worried about what they think is a pterygium but actually have a closely related condition called a pinguecula — a yellowish, slightly raised deposit on the white of the eye that does not extend onto the clear cornea. A pinguecula is even more common than a pterygium, usually causes only mild symptoms if any, and is generally managed with lubricating drops and sun protection rather than surgery. Over time, a pinguecula can develop into a pterygium.
When Do You Need Pterygium Surgery?
Not all pterygia require removal. Many patients with small, stable pterygia are managed conservatively with lubricating drops, anti-inflammatory drops during flare-ups, and sun protection. Surgical removal is recommended when:
- The pterygium is growing toward or threatening the visual axis (central 3mm of the cornea)
- Significant astigmatism is induced, affecting vision
- Chronic irritation and redness are significantly affecting quality of life and are not adequately relieved by drops
- The appearance is a source of significant cosmetic concern to the patient
- Removal is required before cataract surgery, as the pterygium is distorting corneal measurements needed for lens calculation
Surgery is almost always elective, and the timing is agreed between Dr Hunt and the patient based on symptoms and clinical findings.
Does Pterygium Surgery Hurt?
Pterygium surgery is generally a painless day surgical procedure. A specialist anaesthetist provides sedation alongside the local anaesthetic, keeping you comfortable and relaxed during the operation. Dr Hunt and the day surgery team care for you from the moment you arrive until you're ready to go home.
Because the surgery is on the surface of the eye, it is normal to have some mild discomfort and for the eye to look a little red for a while afterwards. This is expected, settles with drops, and is managed at routine follow-up visits.
Why Is a Conjunctival Autograft Important?
Dr Hunt carefully removes the pterygium from the surface of the eye and covers the area with a small piece of healthy tissue taken from under the upper eyelid — a conjunctival autograft. This is the technique with the lowest long-term recurrence rates. The harvest site is not visible, and the eye looks clean and white once everything has settled.
Every pterygium Dr Hunt removes is also sent to the laboratory for examination. The large majority are entirely benign, but occasionally the appearance can hide something more serious such as ocular surface squamous neoplasia (OSSN) — so checking is a routine part of how Dr Hunt handles every case. If anything unexpected is found, management is adjusted accordingly.
What to Expect After Pterygium Surgery
Recovery is usually uneventful. In the weeks after surgery you can expect:
- The eye is often red and mildly irritated for one to two weeks
- Anti-inflammatory and antibiotic drops are used for four to six weeks
- Most patients can return to light work and driving within a few days
- Redness from the graft fades over four to eight weeks; the eye looks white and settled within two to three months
- Sun protection — quality UV-blocking wraparound sunglasses and a broad-brimmed hat when outdoors — is recommended indefinitely to minimise the risk of recurrence
Common Questions
Can a pterygium grow back after surgery?
Recurrence is possible with any technique, but it is significantly less likely when a conjunctival autograft is used — which is why Dr Hunt uses this approach for every pterygium he removes. Ongoing UV protection after surgery also helps reduce the risk.
How long does pterygium surgery take?
The operation typically takes around 30 to 40 minutes. It is performed as day surgery under local anaesthetic with sedation — you go home the same day.
Will removing a pterygium improve my vision?
If the pterygium has induced astigmatism or is encroaching on the visual axis, removing it can improve vision. The corneal surface often takes several weeks to stabilise after surgery, so the full visual benefit may not be apparent immediately.
Can sunglasses prevent a pterygium?
Pterygium develops in response to cumulative ultraviolet exposure over a lifetime — and much of the damage is done in childhood, long before anyone realises the benefits of eye protection. By the time a pterygium appears in adulthood, years of UV exposure have already accumulated. That said, ongoing protection still matters: quality UV-blocking wraparound sunglasses and a broad-brimmed hat reduce further UV load and lower the risk of recurrence after surgery. This is particularly important for people who continue to spend long periods outdoors — whether through work (roofing, landscaping, construction) or recreation (surfing, skiing, sailing).
Is a pterygium dangerous?
A pterygium itself is benign. However, Dr Hunt sends every pterygium he removes to the laboratory for examination, because occasionally the appearance can hide something more serious such as ocular surface squamous neoplasia (OSSN). This is uncommon, but checking is a routine part of how every case is handled.
